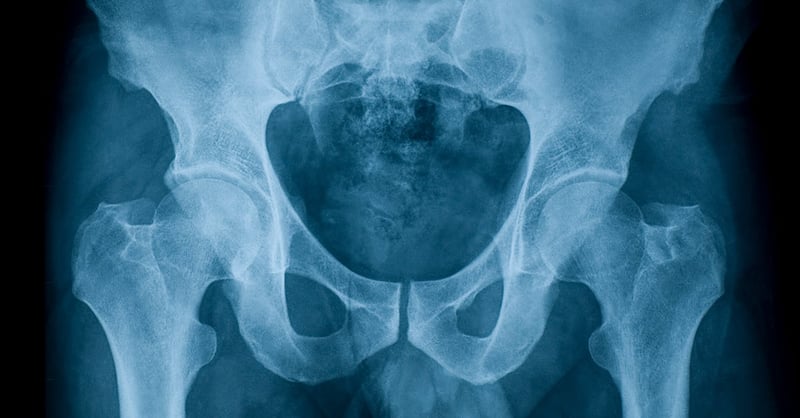
People with physical disabilities often experience hip problems. That said, there are things we can do to improve the development of the hip joint and prevent hip dislocation, also called hip luxation.
We’re delighted to welcome the two Swedish physiotherapists Malin Larsson and Hanna Bengtson, as guest bloggers on the subject of hips. They’ll be addressing the following topics in a three-part series of articles:
- Part 1 – The hip is slipping out of place – so what do we do?
- Part 2 – The hip is slipping out of place – so what do we do?
- Part 3 – Things we can do to benefit hip joint development
The hip is slipping out of place – so what do we do?
So, back to focusing on hips, and back to last week’s insights into how the health and function of the hip joint are affected by the pelvis, the shape of the acetabulum, the angle and appearance of the femoral neck and the pull of the muscles around the hip joint. We also recall that everything from the width of the pelvis to the fit between the acetabulum and the femoral neck, as well as the interaction of the muscles around the hip joint, develops through movement and weight bearing – and so are affected if there’s no movement or weight bearing.
But why is it so important to improve the conditions around the hip joints? What are currently the most common things to be done to prevent hip problems? And what treatments are available when the hip is already slipping out of place? This is what we’re focusing on in the second part of our series of articles on hips. So take a deep breath, because today we’re going to present you with lots of useful facts!
What’s the deal with the hips?
The main reason for hips getting so much attention is simply because it causes so many problems if it luxates (slips out of place), and the risk of that happening is relatively high in people who are not able to stand and walk. Often one and the same person has to deal with all the risk-increasing factors we have mentioned: narrow pelvis, flat acetabulum, femoral neck angled upwards and muscles that is more activated in the direction inward and forward than outward and backward. This creates a situation where the femoral head moves outside the upper edge of the acetabulum over time and eventually ends up outside the joint. This can cause a lot of pain and restrict movement further. As we now know, the hip joint is part of the pelvis, and when the hip is dislocated, the pelvic rim on the same side tilts sharply upwards. This in turn affects the condition of the spine and increases the risk of scoliosis (misalignment of the spine).
If your movement is limited, an appropriate sitting position is essential to enable participation in everyday life. If the person has a dislocated hip, increased pelvic tilt and scoliosis, it can be challenging to find a good and comfortable sitting positing, especially if pain is also an issue.
So, all the X-rays and measurement of range-of-motion, all adjustments of assistive devices, and all those hours of cogitation – that’s what they’re for! Trying to keep that little ball joint within the confines of the acetabulum so as to keep your child moving and limit pain. Sweden is actually a world leader in preventing hip dislocation, but what does that actually involve? And how do we achieve that?
In Sweden they have CPUP which is a Surveillance programme for people with cerebral palsy. You can read more about it here. In Scotland they have corresponding surveillance program called Cerebral Palsy Integrated Pathway Scotland.
What’s usually done to prevent hip dislocation?
Regular check-ups of the hip joints should provide a basis for the best preventive strategy for the situation. Patient autonomy is important in Swedish healthcare, and the proposed strategies are presented as recommendations for you to consider in your capacity as a patient or caregiver. This is an admirable approach in essence, but it’s not uncommon for the feeling of pressure, when you have to make a decision on an intervention suggested for someone you love. What am I actually deciding on? The most common preventive measures offered in Swedish healthcare are described below, along with their purpose and what you can expect. We hope this will give you an idea of the choices you may face.
Some of the interventions mentioned here are based on Swedish guidelines and may therefore deviate from guidelines in your country.
Non-invasive strategies
A strategy is non-invasive if it doesn’t require medical intervention or surgery. These are daily routines that families, childcare services and support groups help out with.
Postural positioning
Aiming for “24-hour postural positioning” is a common concept when it comes to preventing hip dislocation. Postural positioning simply means controlling the position of the torso, pelvis and hips so that the body doesn’t end up in positions that increase the risk of hip dislocation over time. Nowadays, the design of many sitting and standing/walking aids helps to place the user in a neutral position – that is, a position where the torso is upright, the pelvis is guided into a level position and the seat/leg support prevents the legs being pulled inwards and crossing. You can also get specially designed cushions that can help guide the body into a symmetrical position in lying. Collectively, sitting aids, walking/standing aids and positioning cushions provide an opportunity to guide the body into an appropriate position for the joints for much of the 24 hours a day.
Postural positioning can affect the muscles around the hip and, in particular reduce the pull forward and inward of the legs in people with spasticity or without the ability to walk. The purpose is to slow down the process of shortening or “tightening” of these muscles over time. It simply reduces the amount of time the hip joint stays close to its outer position and prevents it from adapting to it. All children with a sparse movement pattern and severely delayed gait onset are offered support with postural positioning aids as part of the treatment.
Effect: Slows the shortening of muscles and avoids outer position of the hip joint.
Axial compression
Axial compression means that the pressure comes directly from the top of the hip joint, as it does when we stand us. When standing upright, the femoral head and the acetabulum are pressed together, which helps the acetabulum to take on its cup-like shape. Standing devices, tilting boards and, to some extent, gait trainers are common aids used to increase weight bearing under axial compression. For the hips, it’s mainly the shape of the acetabulum we want to influence, as well as the angle of the femoral neck towards the acetabulum. All children with a limited voluntary movement and severely delayed gait onset are offered support with standing and walking aids as part of the rehabilitation process.
Effect: Affects the acetabulum and, to some extent, the angle of the femoral neck.
Invasive strategies
An invasive strategy is an intervention or procedure carried out within the framework of healthcare. There’s a lot of new research into hip surgery going on right now, but here are the most common issues you may face as a family member.
Botulinum toxin and baclofen
Botulinum toxin, is a neurotoxin that blocks nerve impulses to the muscle it’s injected into. This is the same thing being used by the beauty industry to iron out wrinkles in foreheads. But for a person living with spasticity, the idea is to shut off the tension in the muscles that are contracting too much in relation to the muscles on the opposite side. When it comes to hip joints, botulinum toxin is injected into the muscles that pull the leg forwards and inwards in order to reduce the pull that places the femoral head in the outer position. Botulinum toxin is considered for people with spasticity when the increased muscle tension is deemed to impede function or the use of assistive devices, or cause pain. The treatment is administered by a doctor, and the aim is to achieve the lowest possible effective dose at intervals, often for four to six months as a cure, because botulinum toxin, like all medicines, has certain side effects and there’s a lack of research into the effects of long-term use on muscles.
Another muscle relaxant is baclofen, which can be administered in tablet form but is sometimes administered via a pump that’s implanted under the skin on the belly and gradually delivers baclofen into the spinal canal so that higher doses can be administered. The aim is the same as with botulinum toxin – to release tension in the muscles that pull the femoral head towards an outer position. That said, baclofen is often used when many of the body’s muscles are so tense that they cause discomfort. Decisions on using botulinium or baclofen are made together with the doctor – usually the child’s neurologist.
Effect: Slows the shortening of muscles and avoids the outer position.
Adductor and psoas tenotomy
The adductors are the muscles that bring the legs together or cross the legs. The psoas is a muscle that draws the leg forward from the hip. A tenotomy is the surgical lengthening of a muscle tendon. So an adductor and psoas tenotomy is an operation to cut and lengthen the muscle tendons that pull the femoral head closer to the outer position. A surgery is an invasive strategy, and although muscles and tendons recover relatively quickly, you should expect a few weeks of pain and limited mobility and at least a few days in hospital. An adductor tenotomy is usually considered when an X-ray shows that almost 50% of the femoral head has moved beyond the edge of the acetabulum. A decision on a tenotomy is made together with the orthopaedist.
Effect: Counteracts the shortening of muscles and avoids the outer position.
Osteotomy
An osteotomy is a surgical procedure that alters the conditions around the hip joint by repositioning the bone itself. Cutting the femur, sawing off a wedge-shaped piece of it, correcting the angle between the femoral head and the acetabulum, turning the knee forward to the correct angle, cutting the pelvis above the acetabulum, inserting the wedge from the femur and fixing everything in place using screws and a plate create new conditions that reduce the risk of hip dislocation. Yes, you read that right. Even if we stop at “cutting the femur”, we realise that this is a major procedure involving pain, restricted mobility and reduced general condition during recovery. And the first few weeks after surgery are often spent on sick leave. An osteotomy is suggested when around 50% of the femoral head is outside the joint, or the patient is deemed to be at high risk of hip dislocation. It’s worth noting that even an osteotomy is viewed as a preventive strategy to avoid hip dislocation, despite the fact that this procedure has a major impact on the person undergoing it. When we say Sweden is a world leader in preventing hip dislocation, we should bear in mind that we have an effective system for monitoring hip joints and are more likely to resort to early osteotomy than many other countries.
Effect: Angle between the acetabulum and the femoral head.
Guided Growth
The Guided Growth Technique, which involves drawing a screw across the growth zone below the femoral neck, is a new strategy for preventing hip dislocation. The aim is to use the screw to alter the direction in which the femoral neck grows and improve the conditions for the hip joint by means of the child’s own growth. This technique has been used for about 50 years to influence knees growing in a knock-kneed or bandy position, but in recent years it’s also proven to be effective in the case of hip joint deformities. The next few years of research will provide lots of important answers, but so far the method seems to have a clear preventive effect on hip dislocation when the femoral head begins to approach 50% outside the acetabulum. Such an intervention presupposes that the child is still growing and doesn’t have constant very high activation of the muscles pulling the legs forward and inward. One positive aspect of the Guided Growth Technique is that it provides relatively easy recovery with major impact on the angle between the femoral neck and the acetabulum over time. You can expect a day or so in hospital and one to two weeks of pain and restricted movement.
Effect: Angle between the acetabulum and the femoral head.
To summarise, we have a good system in Sweden where we closely monitor people at risk of hip dislocation. We receive guidance and assistive devices to influence the hip joints at home, and we have early access to both medication and surgery to nip things in the bud when the hip is slipping out of place, although some surgery can be a tough experience in itself.
If we look at what the most commonly suggested strategies aim to influence, it includes:
- slowing down the shortening of tense muscles
- avoiding outer position of the hip
- the shape of the acetabulum
- the angle between the femoral neck and the acetabulum.
But how do we get the muscles to work and help with development of the pelvis? How do we activate the muscles that stretch, abduct and rotate the hip; muscle work needed to avoid and control the muscles that typically pull the legs forwards and inwards?
Strategies for this aren’t as clearly defined in healthcare, and as a result support in respect of movement and activation of muscles varies widely depending on who’s giving the advice. That’s something we’ll look at more closely in the third and final part of our series of articles focusing on hips! We’ll tell you all about how we work to improve hip health by means of Functional Motor Skills, focusing on movement control and muscle activation.
DON’T MISS IT! (This just happens to be the subject that we’re most passionate about...)

Malin Larsson is a physiotherapist and has a background in sports medicine. Her daughter was born with a disability in 2011, and this inspired her to work with young children and people with disabilities. She’s focused on this field ever since. She began to look at the world through new eyes thanks to her strong little girl facing some major challenges. Malin has been curious to understand basic motor development in depth because of this little girl and her two siblings. She’s gained an insight into just how many people are needed to bring things together to help a child with challenges, and she’s aware that everyone involved needs to have this information presented in different ways if they’re to be able to play their part. Hanna is strongly committed to children’s right to development, to the fact that they should ALL be offered the opportunity to achieve their maximum potential. She’s worked in rehabilitation for more than a decade, working with both children and, adults and has experience of lots of different diagnoses, both congenital and acquired. Taking Functional Motor Skills as her starting point, she wants to get involved and help the network to understand the child’s needs and requirements to help them make progress.
The F-words: Fitness, Function, Friends, Family, Fun and Future help practitioners, educators, and families to create a supportive and...
The Innowalk Pro is an excellent end-effector device, providing full-body robotic therapy in standing with weight-bearing. It can be...
Epilepsy is a serious neurological brain disorder that causes recurring seizures and is common in children with cerebral palsy. There...
Hear from us from time to time and learn new things
