How to preserve healthy bones in individuals with disabilities

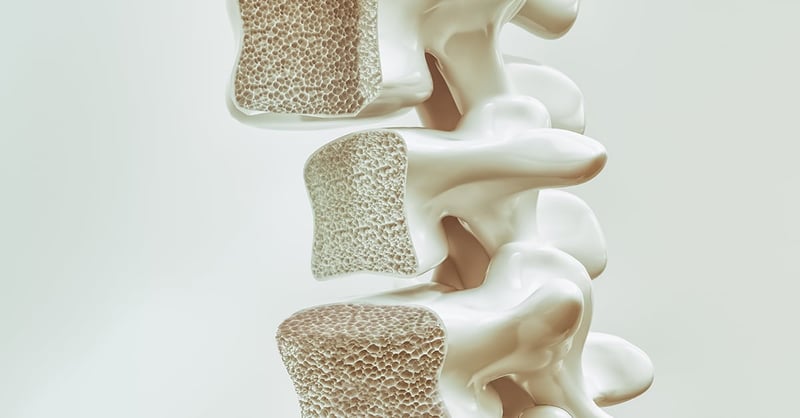
Individuals with physical disabilities have lower bone mineral density (BMD) and are at higher risk of developing osteoporosis compared to healthy individuals. The consequences of low BMD are fractures that occur even without trauma. Why do individuals with physical disabilities have low BMD, and to what extent can we contribute to prevent low BMD and risk of fractures?
- How is bone mineral density measured?
- What causes low bone mineral density (BMD)?
- What might be the consequences of low BMD?
- What can we do to prevent low BMD?
How is bone mineral density measured?
Dual Energy X-ray Absorptiometry (DXA) is the most widely used method for measuring Bone mineral density (BMD). The DXA measures bone mineral content per unit of an area of the body, such as distal femur or whole body. For children, the results are compared with pediatric reference data and adjusted for age, sex and height. BMD is described with a Z-score in children, and a score below 2.0 is considered lower than normal. For adults, the BMD score is described with a T-score. For children, researchers have demonstrated that the most reliable DXA measurements of bone density in children with CP is obtained at the distal femur, because this is the most common site of fractures (Henderson et al 1995).
What causes low bone mineral density (BMD)?
It is well recognized that individuals with physical disability, such as cerebral palsy, are at higher risk of low bone mineral density compared to healthy individuals.
Studies have shown that risk factors for low BMD is:
- Gross motor function level
- Anticonvulsant therapy
- Nutrition
- Calcium intake
- Vitamin D
Gross motor function level
For individuals with cerebral palsy, the Gross Motor Function Classification Scale (GMFCS) act as a predictor for BMD with the most affected groups (GMFCS level IV-V) being 5.7 times more likely to have lower BMD compared to less affected children (GMFCS level I-III). For those individuals who are severely disabled, and who are more prone to having low BMD, the reason is most likely related to limited weight-bearing and mobility. When that is said, it is also important to be aware that a study showed that children with GMFCS II have significantly lower BMD compared to children with GMFCS I (Finbråten et al 2014).
Anticonvulsant therapy
Long term use of anticonvulsant therapy causes changes in calcium and bone metabolism and there is high- to moderate quality evidence showing that epilepsy and the use of anticonvulsants is significantly associated with lower BMD Z-scores.
Nutrition - Calcium - Vitamin D
A great proportion of people with CP have feeding problems and insufficient intake of calcium and vitamin D. Calcium and vitamin D are important nutrients for building strong and healthy bones. Calcium is stored in the bones and teeth and vitamin D are important for calcium uptake. Exposure to sunlight provides the body with vitamin D, but many people with disabilities are spending less time outdoors and might need vitamin D supplement to compensate for this.
What might be the consequences of low BMD?
Low bone mineral density appears in up to 77% of children and adolescents with CP, and nearly 20% of non-ambulatory children and adults will have a femur fracture some time during their life. In children with CP the annual fracture rate is 5% which is twice the rate of what is seen in typically developing children, and 73% of fractures occurred without any documented trauma (Trinh et al. 2015; Han et al. 2016).
As CP life expectancy continues to improve, and bone mass declines with age, it is important to be aware of BMD from early age to prevent low BMD and fractures later in life. Also taking into consideration that over one-third of ambulatory children with CP are at risk for losing the ability to walk in early adulthood, which further increases the risk of low BMD and fractures.
Read also: Why 24-hour posture care management is key
What can we do to prevent low BMD?
The American Academy for Cerebral Palsy and Developmental Medicine (AACPDM) has developed a prevention strategy for children and youth with Cerebral palsy, containing three focus areas:
- Nutrition and Calcium (Ca)
- Vitamin D supplementation
- Weight bearing
When it comes to nutrition and Calcium, the focus should be on following the child's growth chart and be aware of any decrease in weight. Decrease in weight should be avoided as this increases the risk of low BMD. The family might benefit from nutritional counselling to get a better view on what is estimated daily calcium intake and what type of food is recommended to increase calcium intake. Good sources of calcium are for example milk, orange juice, cheese, fish, beans, broccoli, figs, almonds etc. AACPDM have made a nice overview on how much calcium and vitamin D a child needs in relation to age.
Vitamin D supplementation is often needed because the individuals have poor nutrition status and/or little exposed to sunlight. It is recommended to check vitamin D levels before starting up with supplementation and follow up continuously to assure normal range.
Weight bearing is strongly recommended to all individuals with cerebral palsy and should be gained through standing, walking, running and general physical activity. Children, young people and adults who are non-ambulatory should have assistive devices supporting them to be able to stand and/or walk with weight bearing. Mechanical loading through muscle tension and weight bearing loads are important to build and maintain bone density.
Nevertheless you have to be aware that the evidence supporting weight bearing programs as means to improve BMD is not clear. Studies have small sample sizes and are too heterogeneous to draw a conclusion about the efficacy. As for now the best recommendation given is that 60-90 minutes daily standing, 5 days a week can positively affect BMD.
Typically developing children start to pull themselves to standing and bear weight from around 9-10 months of age and take their first steps around 12 months. We should aim for facilitation of standing and walking in children with disabilities at the same age. You as therapist are extremely important in this matter to find an appropriate standing and /or walking device that matches the child’s and the family’s needs. Supporting the family in what they can do together with their child while standing/walking is vital, so this activity is perceived as meaningful for both child and family. Time spent in standing and assuring that it is well incorporated into daily life, is strongly related to comfort and meaningfulness.
Read also: Static or dynamic standing? New study reveals interesting data

Rikke Damkjær Moen brings many years of experience as clinical physiotherapist to the Made for Movement team. Her mission is to ensure that everybody, regardless of mobility problems, should be able to experience the joy and health benefits of physical activity. As our Medical Manager, Rikke is passionate about sharing knowledge so that individuals with special needs, families, and clinicians can discover the possibilities and solutions provided by Made for Movement.
The F-words: Fitness, Function, Friends, Family, Fun and Future help practitioners, educators, and families to create a supportive and...
It's a very special story marked by love, effort, and unstoppable determination. It's about Tom and his family. In the interview,...
A severe accident during a hockey game resulted in 35-year-old Tobias breaking his neck and becoming paralysed from the armpits down....
Hear from us from time to time and learn new things
