Which walking device works best?


Being a pediatric physiotherapist with 35 years of clinical experience, I always look for solutions to improve children’s standing and walking capabilities. To my frustration, it has been difficult to find a walking device that replicates the gait training I facilitate with my own hands during treatment. This triggered me to initiate research and eventually bridging the gap identified with a new type of device. This blog summarizes an oral presentation I did during this year’s EACD conference in Paris.
Improving the potential to ambulate
It’s not easy to give an answer to the question “Which walking device works best” since it depends on the severity of motor disorder and the diagnostic potential to ever be able to walk independently or with support. So for the research I decided to concentrate on CP children GMFCS level I-III where about 70% of the children have the possibility to develop motor control to walk. However, if their gait pattern turns into crouch, ambulation declines over time and 50% of these children will eventually lose their ambulant capacity during adolescence or as young adults.
This group of patients typically have poor motor control, muscle weakness and use a lot of flexion while standing and walking. If untreated, they will develop bone deformities, muscle contractures and the gait becomes inefficient and energy demanding, especially during growth and when increasing body mass. The treatment of this gait pattern is very hard, but can have an effect on the severity of disability. Assistive devices are often used in gait rehabilitation, and I was curious as to which device could give the best results for which type of patients.
In cooperation with the University of Antwerp in Belgium , I did a scopic review on the effect of different walking devices. The conclusions were discouraging. A total of 44 studies on a wide diversity of walking devices showed low level of evidence due to study designs, small sample studies and heterogeneity of population (Lebeer 2019). Further research is needed in all aspects of gait trainer assessment, selection and implementation.
Success criteria in gait rehabilitation
Even if the level of evidence on assistive devices is low, we know from research* that the following factors come into play for successful interventions:
- Early, intensive, task-specific training
- Self-initiated and variability of movements
- Integration into the child’s environment
- Fun and motivating
- Weight- shift and single limb stance
- Trunk stability may improve muscular synergism
My search for a device that facilitates walking with good postural alignment , nice extension of hips and knees and maximal muscle activity of the child was unsuccessful. And I was frustrated to see the patients return to their pathologic pattern when walking outside of therapy with or without a walker. This led me to team up with a multidisciplinary group of people together with the University of Leuven in Belgium to start a feasibility study on a new device - from prototype to end product. The primary objective was to explore if a new device could provide better alignment of the children’s body, improved extensor activity in the lower limbs and weight-shift on one leg to the other without leaning on a saddle or handheld support.
Technical development of a new device started in the field
The feasibility study supported the development of the Hibbot, a gait trainer with adjustable support in six-directional degrees of freedom (DOF). This support is provided by a brace around the lower trunk and pelvis, and is the same support physiotherapists give using their hands around a child’s pelvis, contributing to good upper trunk and head control. In addition, children using the device have a hands-free experience, allowing participation in everyday activities. Training becomes more intensive, fun and on the child’s terms.
The conclusion of this feasibility study was that we had enough insight into applicability and effect to create a guideline for an ongoing study.
Promising results of a recent cross-sectional study
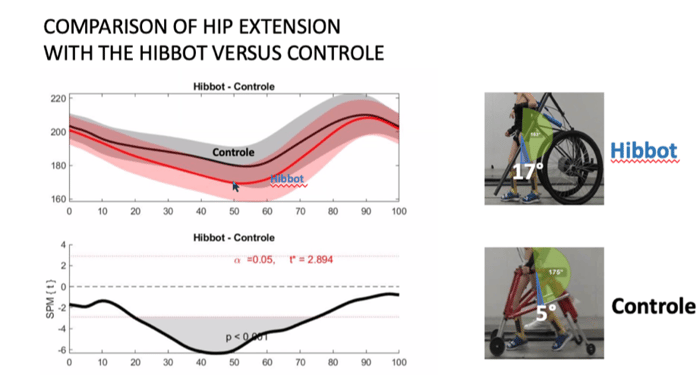
A cross-sectional study was conducted in 2018-2019 where we aimed to compare the gait pattern walking with the Hibbot versus control device on the following parameters:
- kinematics LL and trunk
- temporo-spatial parameters
- video analysis of gait pattern
- ground reaction force
Not all results are official yet, but a significant better hip and knee extension were found walking with the Hibbot in comparison with the control device.
I am very excited to keep working on evidence-based research on the Hibbot and make it a valuable choice in supporting a child’s development. More results from this exciting research will be revealed after we publish an article, so stay put!
If you want more information about the Hibbot, don’t hesitate to contact me.
References
Byrne 2017
Daly 2019
Damiano 2018
Degelaen 2016
Kleim 2008
Lebeer 2019
Hielkema 2019
Morgan 2015
Morgan 2016
Novak 2017
Raid 2015
Smith 2018

Ria Cuppers brings with her over 35 years of experience from clinical practice to the Made for Movement team. She is a dedicated and engaged physiotherapist who has a mission to improve the individual child’s motor capacity in order to be active and participate in everyday life. She focuses on evidence-based methods and includes assistive devices into the rehabilitation perspective to support the child’s development. Ria is the inventor and founder of the new and unique walking device - the Hibbot.
A severe accident during a hockey game resulted in 35-year-old Tobias breaking his neck and becoming paralysed from the armpits down....
A disability entails the loss of, damage to, or deviation from bodily or psychological functions, in the form of mental, physical,...
The Neurological Interdisciplinary Treatment Centre NiB (Neurologisches Interdisziplinäres Behandlungszentrum) is an innovative...
Hear from us from time to time and learn new things
