How Active Standing Improves Physical And Mental Well-Being


In the ongoing mission to develop better treatment strategies for people with physical disabilities, the latest research has begun to shine a bright light onto new approaches to movement therapy.

In particular, the concept of ‘active standing’ is of great interest to many in the field. This is because of a range of potential benefits it promises to offer in countering negative outcomes associated with prolonged sedentary behaviour (SB), affecting ‘many health-related areas such as reflex activity, skin integrity, bowel and bladder function, joint range of motion, and well-being’ (Eng, Levins et al., 2001)
What is Active Standing?
In contrast to a simple static standing position, active standing is considered as low intensity physical activity that elevates an individual's MET rate*. Typically, people with physical disabilities are less active than their peers, and the level of sedentary behaviour (SB) increases in proportion to the level of disability (Verschuren, 2016).
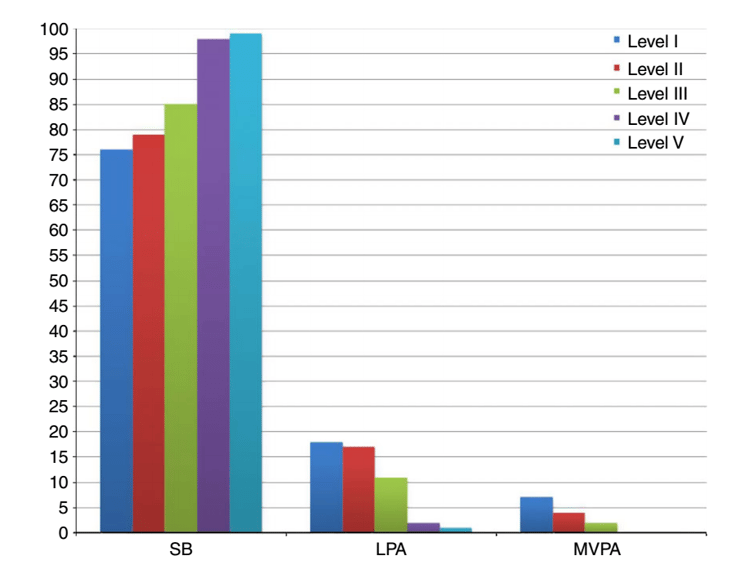
(source: O.Verschuren, M.D. Peterson, A.C.J. Balemans, E.A. Hurvitz, Exercise and physical activity recommendations for people with cerebral palsy, Dev. Med child Neurol., 2016 Feb 7. doi: 10.1111/dmcn.13053)
So, for people with complex physical disabilities, it can be challenging to reach moderate activity levels. However, there is now strong evidence that supports light-intensity physical activity being far healthier for non-ambulatory persons than constant SBs (Verschuren, 2014, 2016). Active standing is therefore a practical approach to getting non-ambulatory people moving at a low-intensity level in order to break everyday SB patterns.
A well-developed active standing strategy will be adapted to the individual, but in general, as a movement therapy, it has three core objectives when trying to engage an individual in new movement or training approaches:
- Training and moving from an upright, standing position with weight-bearing
- Provides maximum muscle stretch and reduces spasticity, muscle deformities and overall muscle activation (Paleg, 2013)
- Allows the individual to experience the joy of physical movement
- Guided, repetitive movements form a corrected position
- Trains coordination of movement patterns in the body
- Reciprocal movements encourages movement patterns between upper and lower body
- Efficient physical training (up to ca. 1500 steps/session)
- Efficient whole-body movement allows for faster progress and more motivation to continue
- Increased activity increases conditions for better participation in everyday activities, both physically and mentally
*MET is the ratio of a person’s working metabolic rate relative to their resting metabolig rate (WHO).
Exploring The Specific Benefits in More Detail
Below we’ve collected the most frequently observed impacts to summarise the most commonly noted benefits of active standing:
- Level of physical activity: because people with disabilities tend to be physically less active than their peers, active standing helps to get non-ambulatory people moving more. This type of movement therapy is not just about interrupting negative health outcomes from prolonged inactivity, but also about inspiring positive change with new patterns of active behaviours. Greater physical participation helps overall health and well-being with better participation in everyday activities (Verschuren, 2014 & 2016)
- Stretching of the muscles and joints: addresses several key areas of sedentary behaviour by improving muscle tone and muscle weaknesses or imbalances, as well as maintaining the range of motion in the lower body (Paleg, 2013)
- Respiration and circulation: being elevated to a standing position extends the trunk more fully, allowing the diaphragm more space in which to expand and contract. This makes breaths deeper and respiration improves overall, also helping to improve the circulatory system; a greater hemodynamic is achieved with active standing in comparison to a static standing position (Glickman, 2010). Active standing also increases physical activity, helping endurance and cardiovascular functioning overall (Verschuren, 2016)
- Greater bone mineral density: non-ambulatory persons are often at risk from low bone mineral density (Henderson, 2002). Active standing encourages greater movement within the muscular system and has been shown to have a positive influence on bone mineral density (Paleg, 2013)
- Gastrointestinal functioning: several studies have noted the stimulation of gastrointestinal functions, particularly in regards to the bowel (Paleg, 2013). It’s thought that stretching of the torso and tilt of the pelvis, in addition to the effect of gravity whilst in an upright position are the biggest factors
- Skin integrity: SB can often mean areas of skin being under constant pressure, compressed by contact with other parts of the body. This can lead to trouble with blood circulation and surface damage such as bed sores. The best way of reducing these risks is to interrupt the SB, thereby relieving pressure on the area and increasing blood circulation (Butler, 2006). The movement promoted by active standing therapy therefore helps to prevent persistent skin integrity problems by relieving areas of constant pressure
- Mental Function: promoting active standing helps to improve mental alertness in individuals by changing their perspective from their usual sitting position. Research has indicated children with Cerebral Palsy scored significantly higher in cognitive testing when stimulated by a standing position in comparison to sitting (Paleg, 2013)
- Social Interaction: last but not least, is the sense of well-being active standing can promote, as it helps create a greater sense of inclusion in the world around the individual. A standing position means being able to communicate at eye level with companions and carers. Studies have observed the positive effects on self-esteem and self-image this can lead to (Pin, 2007)
Breaking SB patterns can be challenging for individuals with physical disability, but all the evidence points to low intensity activity being hugely positive for these individuals. Movement therapy such as active standing can be the answer, providing sensible strategies to break cycles of SBs in a safe, comfortable way for people with limited independent movement. At the heart of basic physical and mental health is the simple need to move the body.
Applying an active standing strategy helps to give people with disabilities the confidence and joy that movement is possible.
References:
- G.S. Paleg, B.A. Smith, L.B. Glickman, Systematic Review and Evidence-Based clinical Recommendation for Doing of Pediatric. Supported Standing Programs, Pediatric Physical Therapy 25(3):232-247, 2013
- R.C. Henderson, R.K. Lark, M.J. Gurka et al; Bone Density and Metabolism in Children and Adolescents With Moderate to Severe Cerebral Palsy, Pediatrics, 2002, vol. 110
- O.Verschuren, V. Leferink, J. Darrah, Muscle activation and energy-requirements for varying postures in children and adolescents with cerebral palsy, J Pediatr. 2014 November; 165(5): 1011-1016
- O.Verschuren, M.D. Peterson, A.C.J. Balemans, E.A. Hurvitz, Exercise and physical activity recommendations for people with cerebral palsy, Dev. Med child Neurol., 2016 Feb 7. doi: 10.1111/dmcn.13053
- C.T. Butler, Pediatric skin care: guidelines for assessment, prevention and treatment, Pediatr Nurs. 2006;32(5):443-450
- T.W. Pin, Effectiveness of static weight-bearing exercises in children with cerebral palsy, Pediatr Phys Ther. 2007 spring;19(1):62-74
- J.J. Eng, S.M. Levins et al: Use of prolonged standing for individuals with spinal cord injury, Physical Therapy Journal, August 2007 81(8): 1392-1399

Rikke Damkjær Moen brings many years of experience as clinical physiotherapist to the Made for Movement team. Her mission is to ensure that everybody, regardless of mobility problems, should be able to experience the joy and health benefits of physical activity. As our Medical Manager, Rikke is passionate about sharing knowledge so that individuals with special needs, families, and clinicians can discover the possibilities and solutions provided by Made for Movement.
The Innowalk Pro full-body movement trainer has been in daily use at the SRH Fachkrankenhaus Neresheim since June 2022. Learn all...
"Alt Movement” in Essex, is an gym for individuals with disabilities. It is an inclusive and welcoming space, where adaptive athletes...
The studyincludedchildrenwith cerebral palsy GMFCS IV and V showedthatseveral hormonal and inflammatorybiomarkersaredysregulated in...
Hear from us from time to time and learn new things
